Why carry out aggressive surgery on the prostate to overcome the symptoms of PBH?

SoracteLite is Elesta Thermotherapy using the ECHOLASER system for treating urinary system disorders (lesions), in particular Benign Prostatic Hyperplasia (BPH).
The name of the treatment contains in a single word a connection with urologic application (“Soracte” is the name of an Italian mountain (also named in the incipit of an Horace Poem) where there was a monastery in which the monk Nonnoso, canonized, is considered the protector of people with kidney disease) and “Lite”, which on one hand refers to the lightweight and micro-invasiveness of the treatment, and on the other, the therapeutic source (Light, therefore Laser).
The name SoracteLite allows for differentiating the procedure with ECHOLASER (micro-invasiveness and multi-fibre approach in a single system) from the other thermal ablation techniques
Indications
SoracteLite is indicated in the case of patients suffering from Benign Prostatic Hyperplasia, a disease in which the volumetric increase in the prostate gland generates a compression effect at the level of the bladder floor and the urethral canal, and also in the case of subjects who choose not to undergo surgical treatment.
When you hear the word laser in urology, you instantly may think of surgical lasers, like the green laser. These lasers are an important advancement for endoscopic, transurethral surgery of the prostate. However, SoracteLite has got nothing to do with surgical lasers; in fact, it differs in wavelength and power (our laser is not visible as opposed to green), its mode of action (cytoreduction vs surgical vaporization), and lastly and most importantly SoracteLite is performed in a truly microinvasive approach (transperineal vs transurethral). SoracteLite represents true innovation for BPH treatment.
Despite focusing mainly on the treatment of Benign Prostatic Hyperplasia (BPH), SoracteLite is also effective for prostate cancer that is not clinically relevant combined with active surveillance and post-prostatectomy relapse and for kidney cancer.
Performance
- shrinkage of the enlarged prostate volume due to BPH with consequent gradual and steady relief from symptoms based on Laser Induced CytoReduction (LICR) process;
- complete ablation of malignant tumours, with a sufficient safety margin
What is it?
SoracteLite treatment consists of the percutaneous insertion of optical fibres (one or two fibres per lobe depending on the basal volume of the prostatic gland) via transperineal access, and the delivery of laser energy for several minutes which causes the heating of the tissues until they are destroyed, followed by a progressive reduction in the volume of the prostatic lobe (a reduction of at least 40% compared to the basal volume at the one-year follow-up) and subsequent disappearance of the symptoms. The planning of the treatment, the insertion of the needles and the monitoring are all carried out under ultrasound guidance. In order to facilitate the insertion manoeuvre, the system has a dedicated multi-applicator Guiding System for transrectal ultrasound probe with relative Biopsy Software that displays the guidelines on the screen.
With just one SoracteLite session it is possible to have a significant and persistent reduction in the volume of the prostatic gland and disappearance of the local symptoms, without changing the physiology of the prostatic gland.
Clockwise:
1. TRT33 Esaote Probe with multi-fibre guiding system / 2. Multi-fibre Biopsy Software
3./4. TRT33 Esaote Probe equipped with multi-fibre guiding system
Advantages
- resolution of symptoms
- “in situ” thermal damage with consequent reduction of the prostatic lobe
- preservation of the healthy tissue and the organ function
- highly predictable and repeatable coagulation volume
- use of fine, a-traumatic needles with transperineal approach
- absence of general anaesthesia
- short duration of the treatment (few minutes)
- rapid recovery times
- no or insignificant post-treatment pain
- absence of erectile dysfunction or complications linked to the reproductive organs
Clinical Case no.1
Patient suffering from BPH, with a basal volume of 64 ml. Treated with two fibres per lobe.
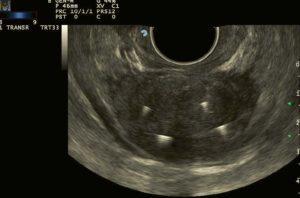
US image before treatment
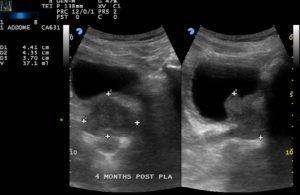
Four-month follow-up US image
The four-month follow up revealed the following:
- volumetric reduction from 64 ml to 37 ml
- post-urination residue reduction from 200 ml to 43 ml
- IPSS score reduction from 29 to 10
- Quality of Life (QoL) from 5 to 1
- Maximum flow speed up from 4 ml/s to 14 ml/s
- Absence of complications
Images by courtesy of Dr. Patelli (Pesenti Fenaroli Hospital, Alzano Lombardo)
Transperineal Laser Ablation for Percutaneous Treatment of Benign Prostatic Hyperplasia: A Feasibility Study
Patelli G, Ranieri A, Paganelli A, Mauri G, Pacella CM
Cardiovasc Intervent Radiol (2017). doi:10.1007/s00270-017-1662-9
Tolerability of percutaneous ablation Neodymium Laser in patients suffering from Benign Prostatic Hyperplasia (BPH): Prospective Observational Pilot Study
- No. of patients enrolled: 10
- Reference Study Centre: Pesenti Fenaroli Hospital, Alzano Lombardo (BG)
- Promoter: Dr. Gianluigi Patelli
- Study Status: Terminated
10 reasons to choose SoracteLite Echolaser for treating urinary system disorders (lesions), in particular Benign Prostatic Hyperplasia (BPH)
1. SoracteLite treatment ensures the resolution of the symptoms
SoracteLite gives rise to the disappearance, or in any case the reduction, of the local symptoms due to the compression exerted by the enlarged prostate lobes to the initial urethral tract and the lower part of the bladder, thus ensuring a substantial recovery of patient’s quality of life.
2. SoracteLite treatment allows “in situ” thermal damage with consequent reduction of the prostatic lobe
One or two fibers are inserted in each prostatic lobe through extremely fine needles (21 G < 0.8 mm) under US guidance, in order to have a real-time feedback of the treatment. Echolaser is a multi-source system that allow to use from one to four laser sources simultaneously, giving the operator the possibility to perform different coagulation areas, in relation to the prostate basal volume (even for prostates > 100 gr)
3. SoracteLite treatment allows the preservation of the healthy tissue and the complete organ function
One of the main differences of SoracteLite treatment with respect to other mini-invasive techniques is that there is no direct tissue removal. The coagulation of tissue is performed within the prostate lobe, than the reduction process of the lobe occurs due to transformation and natural body reabsorption of the treated tissue. This leads to a reduction in pressure of the prostatic urethra which relieves the patient symptoms. The maximum effect is reached a few weeks after the treatment.
4. SoracteLite treatment ensures highly predictable and repeatable coagulation volume
The laser energy delivered through the optical fibers give rise to a coagulation zone with highly predictable volume thanks to the localised effect of the laser source, thus allowing the operator to treat only the desired portion of tissue, preserving the structures situated near the prostate lobes, such as the urethral channel and the bladder
5. SoracteLite treatment is performed through the use of fine, a-traumatic needles with transperineal approach
The use of extremely fine needles (21 G) and the transperineal approach, lead to several advantages such as:
- No risk of bleeding
- No risk of infections (no removal of tissue and no interactions with urinary structures)
- No risk of sexual complications
- No complications to the urethra
Moreover, in contrast to the more common transurethral approach, sonographic-controlled, perineal interstitial laser therapy keeps the operator constantly informed (transrectal ultrasound) about the exact position, i.e. the actual depth of the laser fiber tip. The transurethral approach cannot supply this detailed information and therefore cannot offer this distinct advantage
6. SoracteLite treatment is performed in absence of general or spinal anaesthesia
The operator performs only local anaesthesia in the periprostatic plexus and perineal skin, leaving the patient conscious and able to directly interact with the physician during the procedure, increasing the safety and ensuring the correct performance of the treatment. Moreover this feature allow to treat all the patients that cannot undergo general or spinal anaesthesia
7. SoracteLite treatment allows to treat high prostatic volumes
SoracteLite treatment allows to treat prostates with high basal volumes (even > 100 ml), thanks to the multi-fiber approach and to a special technique called pull-back, in which the operator can perform more than a single illumination in a single treatment, pulling back the needles and fibers for about 1 cm after each deposition of energy. Using that particular technique the physician can increase the coagulation volume within the prostate lobe. Hereafter are reported the mean prostate volumes that can be treated with the different techniques:
- TUIP (transurethral incision < 30 gr )
- TURP ( transurethral resection < 80‐100 gr )
- LASER (transurethral 80‐100 gr ) LASER (SoracteLite, transperineal > 30 gr)
- OPEN ( prostatectomy 80‐100g)
8. SoracteLite treatment allows fast treatment times
The treatment duration varies in relation to the prostate basal volume, from a minimum of 10 minutes to a maximum of 30 minutes for prostates with basal volumes > 100 ml. Rapid treatment times are also allowed thanks to the excellent conversion of the laser energy into thermal energy, that produces the coagulation area.
9. SoracteLite treatment allows rapid recovery times
The patient is dismissed and can return to his normal activities the day after the treatment. During the period following the procedure the patient will have to undergo ultrasounds follow-up exams to evaluate the reduction of the volume of the prostate lobes
10. Complications and side effects after the procedure
- Retrograde ejaculation
- Dysuria (several weeks after the procedure)
- Transient urinary incontinence
- Infections of the urinary tract
- Urethral stenoses
- Irritating urinary symptoms (urination might be painful, a sense of urgency or frequent need to urinate from 6 to 8 weeks after treatment)”



